Study shows how brain tumors make certain immune cells turn rogue
Ludwig Institute for Cancer Research | 09-27-2023
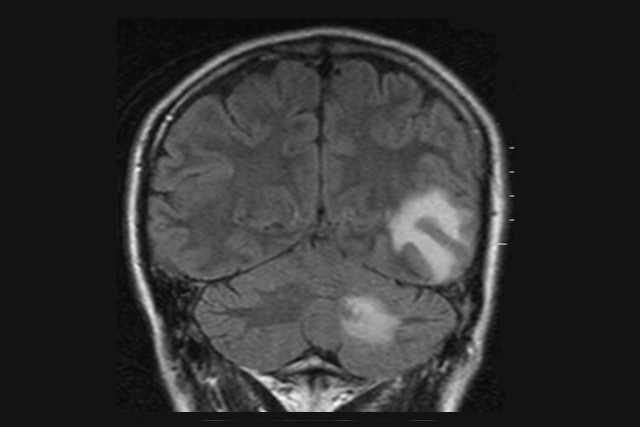
A Ludwig Cancer Research study has for the first time exhaustively analyzed immune cells known as neutrophils that reside in brain tumors, including gliomas, which develop in the brain itself, and cancers that spread there from the lung, breast and skin.
Led by Ludwig Lausanne’s Johanna Joyce and Roeltje Maas, an MD-PhD student in her laboratory, the study also details the key role neutrophils play in ensuring the survival of brain cancers and exposes the mechanisms by which the tumor microenvironment (TME) tweaks their biology to turn them into enablers of malignant growth. Its findings suggest new approaches to the treatment of both gliomas and brain metastases (BrMs).
“Our study shows for the first time how the brain tumor microenvironment draws in and disarms infiltrating neutrophils, stretches out their lifespans—which are otherwise relatively short—and turns them into cells that suppress anti-cancer immune responses while directing the generation of blood vessels that feed the growing cancer,” said Joyce.
Reported in Cell, the study interrogates the preferential spatial niches, dynamics, gene expression patterns and functional states of neutrophils in BrMs and gliomas. Notably, it identifies specific cellular interactions and a pair of molecular factors in the TME that are key to converting neutrophils from potential agents of anti-tumor immunity into abettors of malignancy.
“This is one of the most exciting discoveries of the study because only a small subset of brain metastases respond to currently available immunotherapies, and gliomas have proved especially resistant to all types of treatment,” said Maas. “Our identification of specific cellular and molecular factors that can turn neutrophils into immunosuppressive and pro-tumoral agents in the TME opens the door to developing therapeutic approaches to make brain cancers more susceptible to immunotherapy.”
Cancers depend on a menagerie of noncancerous cells to survive and thrive, and brain tumors are no exception. In exploring this aspect of brain cancer biology, the Joyce lab has in recent years extensively analyzed the immune landscape of gliomas and BrMs, identifying new strategies to address their recurrence and resistance to therapy.
Much of that work has focused on myeloid immune cells, most notably macrophages and their brain-resident versions known as microglia. Joyce and her colleagues observed in these studies that neutrophils—which are also myeloid cells—accumulate in large numbers in brain tumors, especially in the most aggressive types of gliomas and BrMs, raising questions about their potential role in tumor progression.
The current study answers those questions. Based on an integrated, multifactorial analysis of more than 190 brain tumor samples from patients and experiments in a variety of mouse models of brain cancer, it shows that neutrophils are more abundant in BrMs than in primary gliomas. In all tumor types, however, their phenotypes—or physical traits and functional states—differ significantly from those of neutrophils in the circulation and in healthy brain tissues.
Maas, Joyce and colleagues report that tumor-associated neutrophils (TANs) tend to cluster around the malformed and leaky blood vessels in tumors and switch off gene expression programs that induce cell death while turning on genes that support cell survival—thus lengthening their lifespans. These findings were confirmed in pioneering studies performed in mouse models of brain cancer.
Once ensconced in the TME, the researchers found, TANs start churning out factors that stimulate the formation of blood vessels. They also become functionally suppressed, halting the production of reactive oxygen species—the molecular bomblets neutrophils ordinarily use to destroy their cellular targets.
But TANs, it turns out, aren’t just victims of immunosuppression. They’re also its perpetrators. The researchers show that TANs clustered around tumor blood vessels associate with and apparently suppress cytotoxic T cells—the frontline forces of the immune system that kill cancer cells and are engaged by most approved immunotherapies.
Maas, Joyce and colleagues identify multiple factors that recruit TANs into the TME and induce their functional transformation. Two inflammatory factors, however, seem to be critical: the signaling molecule TNF-α and ceruloplasmin, a copper-carrying protein. Both, the researchers show, are produced by neutrophils themselves as well as macrophages and microglia.
“This adds to growing evidence that the myeloid niche of the tumor microenvironment is central to the establishment and maintenance of a profoundly immunosuppressive microenvironment across brain tumor types that supports the survival and progression of these generally lethal cancers,” said Joyce.
She and her colleagues will now examine whether targeting the inflammatory factors and cellular interactions that induce TAN immunosuppression can help improve brain tumor responses to immunotherapy.
Source:
Materials provided by the Ludwig Institute for Cancer Research. Content may be edited for clarity, style, and length.