Role of T cells in Alzheimer’s related diseases suggests new treatment strategy
Washington University School of Medicine | 03-08-2023
Nearly two dozen experimental therapies targeting the immune system are in clinical trials for Alzheimer’s disease, a reflection of the growing recognition that immune processes play a key role in driving the brain damage that leads to confusion, memory loss and other debilitating symptoms.
Many of the immunity-focused Alzheimer’s drugs under development are aimed at microglia, the brain’s resident immune cells, which can injure brain tissue if they’re activated at the wrong time or in the wrong way. A new study from researchers at Washington University School of Medicine in St. Louis indicates that microglia partner with another type of immune cell — T cells — to cause neurodegeneration.
Studying mice with Alzheimer’s-like damage in their brains due to the protein tau, the researchers discovered that microglia attract powerful cell-killing T cells into the brain, and that most of the neurodegeneration could be avoided by blocking the T cells’ entry or activation. The findings, published March 8 in the journal Nature, suggest that targeting T cells is an alternative route to preventing neurodegeneration and treating Alzheimer’s disease and related diseases involving tau, collectively known as tauopathies.
“This could really change the way we think about developing treatments for Alzheimer’s disease and related conditions,” said senior author David M. Holtzman, MD, the Barbara Burton and Reuben M. Morriss III Distinguished Professor of Neurology. “Before this study, we knew that T cells were increased in the brains of people with Alzheimer’s disease and other tauopathies, but we didn’t know for sure that they caused neurodegeneration. These findings open up exciting new therapeutic approaches. Some widely used drugs target T cells. Fingolomid, for example, is commonly used to treat multiple sclerosis, which is an autoimmune disease of the brain and spinal cord. It’s likely that some drugs that act on T cells could be moved into clinical trials for Alzheimer’s disease and other tauopathies if these drugs are protective in animal models.”
Alzheimer’s develops in two main phases. First, plaques of the protein amyloid beta start to form. The plaques can build up for decades without obvious effects on brain health. But eventually, tau also begins to aggregate, signaling the start of the second phase. From there, the disease quickly worsens: The brain shrinks, nerve cells die, neurodegeneration spreads, and people start having difficulty thinking and remembering.
Microglia and their role in Alzheimer’s have been intensely studied. The cells become activated and dysfunctional as amyloid plaques build up, and even more so once tau begins to aggregate. Microglial dysfunction worsens neurodegeneration and accelerates the course of the disease.
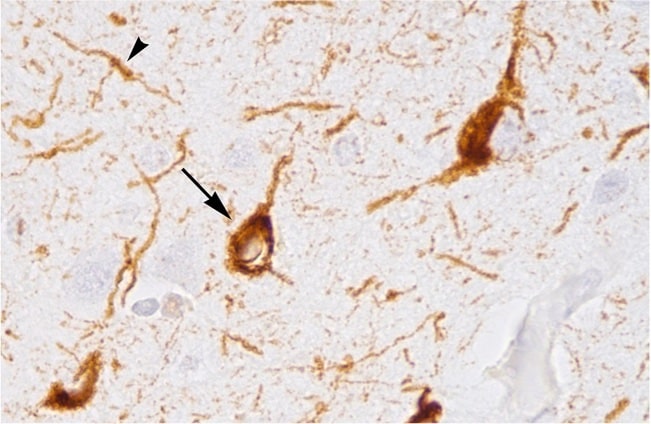
First author Xiaoying Chen, PhD, an instructor in neurology, wondered about the role of other, less studied immune cells in neurodegeneration. She analyzed immune cells in the brains of mice genetically engineered to mimic different aspects of Alzheimer’s disease in people, looking for changes to the immune cell population that occur over the course ofThis photomicrograph the disease.
Mirroring the early phase of the disease in people, two of the mouse strains build up extensive amyloid deposits but do not develop brain atrophy. A third strain, representative of the later phase, develops tau tangles, brain atrophy, neurodegeneration and behavioral deficits by 9½ months of age. A fourth mouse strain does not develop amyloid plaques, tau tangles or cognitive impairments; it was studied for comparison. Along with Chen and Holtzman, the research team included Maxim N. Artyomov, PhD, the Alumni Endowed Professor of Pathology & Immunology, and Jason D. Ulrich, PhD, an associate professor of neurology, among others.
The researchers found many more T cells in the brains of tau mice than the brains of amyloid or comparison mice. Notably, T cells were most plentiful in the parts of the brain with the most degeneration and the highest concentration of microglia. T cells were similarly abundant at sites of tau aggregation and neurodegeneration in the brains of people who had died with Alzheimer’s disease.
Additional mouse studies indicated that the two kinds of immune cells work together to create an inflammatory environment primed for neuronal damage. Microglia release molecular compounds that draw T cells into the brain from the blood and activate them; T cells release compounds that push microglia toward a more pro-inflammatory mode.
Eliminating either microglia or T cells broke the toxic connection between the two and dramatically reduced damage to the brain. For example, when tau mice were given an antibody to deplete their T cells, they had fewer inflammatory microglia in their brains, less neurodegeneration and atrophy, and an improved ability to perform tasks such as building a nest and remembering recent things.
“What got me very excited was the fact that if you prevent T cells from getting into the brain, it blocks the majority of the neurodegeneration,” Holtzman said. “Scientists have put a lot of effort into finding therapies that prevent neurodegeneration by affecting tau or microglia. As a community, we haven’t looked at what we can do to T cells to prevent neurodegeneration. This highlights a new area to better understand and therapeutically explore.”
Source:
Materials provided by Washington University School of Medicine. Content may be edited for clarity, style, and length.
